
We are now accepting volunteer applications for our upcoming 25th Annual Century Group Delta Health Classic Golf Tournament >>
What does a day in the life of an ER physician look like?
You can always tell the tone of the shift when you walk in, from the tone of the waiting room and the expression on your charge nurse’s face. Our ER physician team is also the code blue response team for the hospital. One second you might be quickly reassessing a wound then there’s an overhead page for a code blue you need to respond to.
Our ER department is also a popular training site for UBC Faculty of Medicine, and we often have medical students and residents who rotate through our department. So while we also see patients, we are reviewing patients with our learners and teaching based on the cases on shift.
Can you tell us about our ER?
Over the past decade, the ER volumes have gone up 30%, resulting in a corresponding increase in daily physician hours. The Delta Hospital ER was the first community emergency department in Canada to be designed with negative pressure capacity. The acute care zone includes a resuscitation bay and ten telemetry or cardiac monitored beds. The non acute zone includes two negative pressure rooms along with fast track bays for suturing and casting along with rooms for eye exams and gynecological exams.
The ER also contains an observation unit which was used pre-COVID for admitted patients waiting for ward beds, outpatient antibiotics and non-urgent issues. Since the start of the pandemic, the observation unit has been converted to a ‘hot’ zone for patients with COVID concerns. This zone has upgraded bedside telemetry monitors courtesy of the Foundation funding which will enable greater monitoring capacity during and after the pandemic.
Thanks to our generous donors, the Foundation is able to purchase priority equipment for the ER. Can you tell us what this support means to your department?
Having the most state-of-the-art technology and equipment is vital to a modern ER. Some of the items purchased this year with donor dollars include a transport defibrillator, an ultrasound, suture station, and a hyperthermia blanket system.
Upon the onset of the pandemic, donor generosity and Foundation support has also allowed rapid procurement of equipment specifically related to COVID. The equipment has enabled the ER to focus on learning new protocols and procedures during weekly simulation sessions and supporting each other as a team during the pandemic’s initial stages. The ER team feels reassured that we are equipped to deal with any resurgent cases and this year’s upcoming influenza season. Beyond the monetary generosity, the ER staff felt the community’s support and commitment during this stressful and trying time. We are honoured the Foundation and its donors are so passionate and continue to ensure quality care through pandemic or non-pandemic times.
How has COVID-19 changed THE WAY the ER functions?
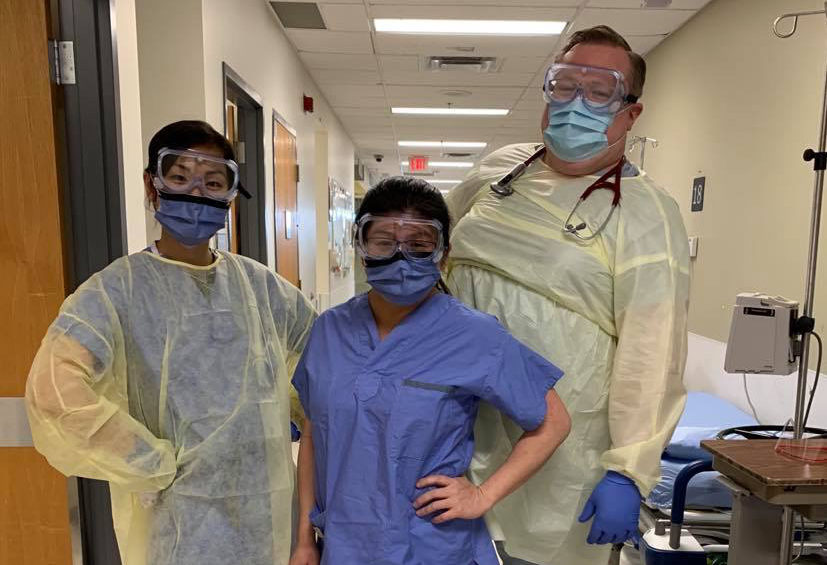
The ER’s two negative pressure rooms have been in continuous use since the start of the pandemic for COVID testing, isolation and resuscitation. The emergency team spent hours redesigning the patient journey to ensure proper isolation procedures and social distancing for staff and patients while continuing to care for acutely ill patients. Patients will notice additional front door screening, and upgraded infection control and isolation procedures. Personal protective equipment (PPE) is taken seriously to minimize transmission between patients and to ensure staff safety. ER staff now don full face masks with eye protection and hospital scrubs for their shift. This is used for procedures with potential airborne transmission such as intubation, positive pressure ventilation or conscious sedation.
We anticipate that the upgraded infection control measures will continue as the ‘new normal’. This has meant that procedures that can potentially cause airborne transmission need to be performed in enclosed rooms.